The Freckle That Turned Out to Be Vulvar Cancer: Would you know the signs?
Scrolling through TikTok as one does, a video came across my FYP or “for you page” – it was a woman talking about the fact that she just found out that this tiny freckle on her vulva turned out to be vulvar cancer. She was now devastated and terrified and facing surgery. She was bravely sharing her personal story, as so many thankfully do on TikTok, to offer information that might save someone else’s life.
You can view her TikTok here. Kimberley (@kdhay15) | TikTok
@kdhay15 My main point of sharing this is I never knew that I was supposed to look at myself, and I am believing that this is a very very early detection, which is what we want, but I would not have found it unless I did it myself. Pap smear does not diagnose this and most doctors just go go quick and swab you you need to move your junk and look at yourself.#cancer ♬ original sound – Kimberley
She Almost Missed It
This woman is in her 50s, the age when vulvar cancer becomes more prevalent, and had, like far too many women, never looked at her vulva in any real detail. (That topic is another article I will write because it is crazy to me that so many women (or their doctors!) don’t look at their vulvas as part of regular self-care.)
And because doctors rarely if ever inspect your vulva when doing a gynecological exam and her partner had passed a few years back, no one else had intimate knowledge of her nether regions and noticed a change.
In her case, she said it was a freckle that “wasn’t there before.” No itching, no redness, no lump. Just a freckle that was out of place.She mentioned it to her GYN and they decided to take a biopsy and it came back positive for vulvar cancer.
Vulvar Cancer is Rare but Not As Uncommon As I Had Thought
After reading through the comments on her video, I realized that I had no idea how common this cancer was for so many women. The entire comment section was story after story of women dealing with vulvar cancer. I put the hashtag ‘#vulvar cancer’ into the search bar on TikTok, and I was flabbergasted at the sheer number of videos of women and doctors talking about their experiences with this cancer. I am 63 and well educated, not a pushover at my doctors and I research everything for a living and I had not been aware of this form of cancer and that I should be doing self exams for it.
Time To Do A Little Research
I went to do a little research through the authoritative medical and science resources online to give you and me a short primer on vulvar cancer. Take 5 minutes to read this. Grab a hand mirror and learn to conduct regular self-exams. It may save your life.
For more in-depth information, all information sources are at the end of this overview. Please always speak with your health care team if you have any questions or concerns. This overview is for informational purposes only.
Understanding Vulvar Cancer: Prevalence, Symptoms, and Treatment Options
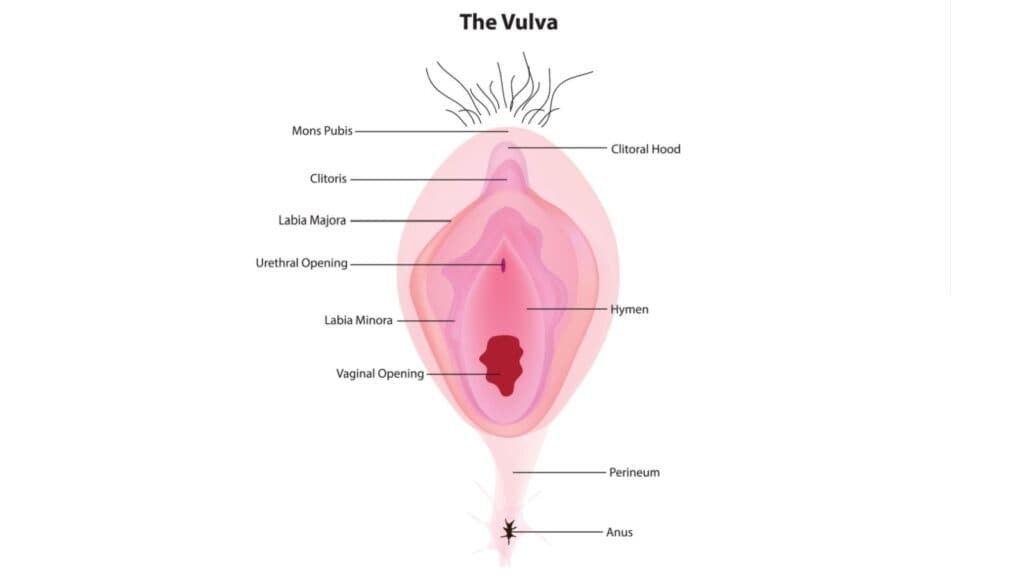
Vulvar cancer, a rare but significant gynecological malignancy, affects the external female genitalia, known as the vulva. This comprehensive overview draws on authoritative sources to explore the prevalence, symptoms, treatment options, and signs of vulvar cancer, providing essential information for awareness and management.
Prevalence of Vulvar Cancer
Vulvar cancer accounts for about 0.3% to 0.7% of all cancers in women, with approximately 6,400 new cases diagnosed annually in the United States. It primarily affects older women, particularly those aged 65 and above, although it can occur at any age. The incidence of vulvar cancer has been relatively stable over time, but it remains a concern due to its impact on women’s health.
Symptoms and Signs of Vulvar Cancer
The early stages of vulvar cancer may not present any symptoms, making early detection challenging. However, as the disease progresses, several signs and symptoms can manifest, including:
- Persistent itching, burning, or pain in the vulva.
- Changes in the color or thickness of the vulvar skin, which may appear redder or whiter than normal.
- The presence of a lump, wart-like growths, or ulcers on the vulva that do not heal.
- Bleeding or discharge not associated with menstrual periods.
- Pain during urination or sexual intercourse.
These symptoms are not exclusive to vulvar cancer and can be caused by other, less serious conditions. However, persistent changes should prompt a consultation with a healthcare provider for proper diagnosis and management.
Diagnostic Approaches
Diagnosing vulvar cancer typically involves a physical examination of the vulva, possibly using a magnifying device to inspect the area better. A biopsy, where a small tissue sample is removed for laboratory analysis, is crucial for confirming the presence of cancer cells.
Treatment Options for Vulvar Cancer
The treatment of vulvar cancer depends on the stage of the disease, the size of the tumor, and the patient’s overall health and preferences. The main treatment options include:
Surgery
Surgery is the cornerstone of treatment for vulvar cancer, aiming to remove the cancerous tissue while preserving as much normal tissue as possible. Types of surgeries include:
- Wide local excision : Removal of the tumor and a margin of healthy tissue.
- Radical vulvectomy : Removal of the entire vulva in cases of extensive cancer.
- Sentinel lymph node biopsy : To check for the spread of cancer to lymph nodes.
Radiation Therapy
Radiation may be used before surgery to shrink large tumors or after surgery to eliminate any remaining cancer cells. It can also be an option for patients who are not surgical candidates.
Chemotherapy
Chemotherapy is typically reserved for advanced cases or when the cancer has recurred. It can be used alone or in combination with radiation therapy.
Chemoradiation
A combination of chemotherapy and radiation therapy may be used for more aggressive cases or for tumors that have spread to the lymph nodes.
Coping and Support
Living with vulvar cancer can be physically and emotionally challenging. Patients are encouraged to seek support from healthcare providers, counselors, or support groups. Education about the disease and its treatment can also help patients make informed decisions about their care.
Conclusion
Vulvar cancer, while rare, requires attention due to its potential impact on a woman’s health. Awareness of the symptoms and early consultation with a healthcare provider can lead to timely diagnosis and effective management. Many women can manage this disease and maintain a good quality of life with appropriate treatment.
If you have any concerns or questions be sure to speak with your health care provider.
Citations:
- https://www.cancer.net/cancer-types/vulvar-cancer/types-treatment
- https://www.cancer.org/cancer/types/vulvar-cancer/treating.html
- https://www.nhs.uk/conditions/vulval-cancer/treatment/
- https://www.ncbi.nlm.nih.gov/books/NBK567798/
- https://www.mayoclinic.org/diseases-conditions/vulvar-cancer/diagnosis-treatment/drc-20368072
- https://www.cedars-sinai.org/health-library/diseases-and-conditions/v/vulvar-cancer-overview.html
- https://www.moffitt.org/cancers/vulvar-cancer/faqs/what-are-the-warning-signs-of-vulvar-cancer/
- https://www.nhs.uk/conditions/vulval-cancer/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8773873/
- https://www.hopkinsmedicine.org/health/conditions-and-diseases/vulvar-cancer
- https://www.cancer.org/cancer/types/vulvar-cancer/detection-diagnosis-staging/signs-symptoms.html
- https://www.cancer.gov/types/vulvar/hp/vulvar-treatment-pdq
- https://www.mayoclinic.org/diseases-conditions/vulvar-cancer/symptoms-causes/syc-20368051
- https://my.clevelandclinic.org/health/diseases/6220-vulvar-cancer
- https://www.cdc.gov/cancer/vagvulv/basic_info/symptoms.htm
- https://www.cancer.org.au/cancer-information/types-of-cancer/vulvar-cancer
- https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/vulval-cancer
- https://www.cancer.net/cancer-types/vulvar-cancer/statistics
- https://www.cancer.net/cancer-types/vulvar-cancer/introduction
- https://www.cancer.gov/types/vulvar/patient/vulvar-treatment-pdq
Join Us

Join us on this empowering journey as we explore, celebrate, and elevate “her story.” The Queen Zone is not just a platform; it’s a community where women from all walks of life can come together, share their experiences, and inspire one another. Welcome to a space where the female experience takes center stage. Sign up for our newsletter so you don’t miss a thing, Queen!